By now we should have all heard the news. The novel coronavirus, recently labeled by the WHO as COVID-19 (COrona VIrus Disease 2019), outbreak has caused more deaths than SARS and continues to have a growing incidence of infection in the US. In fact on January 30, 2020 the WHO declared the outbreak a public health emergency of international concern (PHEIC). As expected patients are scared and are bound to get worried. They have already started to bring up concerns along the lines of “Doctor, I am worried I have the coronavirus.” How do you want to respond? The goal of this post is to simply make sure we, as residents, can formulate a prepared response for our patients and have a basic management approach when deemed necessary.
How bad is the outbreak? (updated 2/11/20)
Since 12/31/2019 and as of 2/11/2019, the current novel coronavirus outbreak is worldwide with 43.1k confirmed cases, of which 42.7k are in China. There have been 1017 deaths recorded, of which only one is outside of China. In comparison, the influenza virus is still more of a threat, especially in the US, with 15 million illnesses worldwide, 140k hospitalization and 8k deaths.

More updated info can be found via the daily WHO situation reports.
What is the difference between COVID-19 and SARS?
SARS (Severe Acute Respiratory Syndrome) was a well known coronavirus outbreak originating in the 2003 that also originated in China. In order to provide a simple response to your patients that does not drive too much into virology, understand that genome sequencing to date shows that both COVID 19 and the SARS virus originated from a similar coronavirus subtype and might have the same structure for receptor-binding. Both also appear to have been traced back to bats as the primary source but the intermediate host has yet to be determined. In its severe setting, both cause death through complications from progressing to acute respiratory distress syndrome (ARDS).
When should you suspect COVID-19 infection?
Characterized by the usual viral symptomatology, COVID-19 presents most frequently with viral pneumonia symptoms including fever, cough, dyspnea and bilateral infiltrates on chest Imaging. Less common symptoms include sore throat, sputum production, headache, hemoptysis and diarrhea. However this is quite variable as a virus presents on a spectrum of disease and varies by the severity of illness and age, ranging anywhere from asymptomatic to severe disease that includes respiratory failure, shock, organ failure and ARDS requiring intensive care. Those at risk for severe disease include the elderly, those with comorbid conditions and the verdict is still out on those in contact with farm animals. The most important risk factor that should raise suspicion of infection is the epidemiological risk i.e. those whom, within 14 days, have had close contact with someone who had a laboratory-confirmed infection or themselves have a recent travel history to one of the affected regions in China. The CDC presents clinical criteria for patients under investigation however we anticipate that these recommended criteria will be adjusted as more data is made available.

When suspected these are the patients that you should obtain a diagnostic workup and implement the immediate infection control measures discussed below.
How do you diagnose COVID-19 infection?
Simply stated, you report it. When you have a PUI for COVID-19 based on the above criteria as outlined by the CDC, notify the infectious control personnel at our health care facility: they will work with the State Health Department or CDC for the diagnostic eval. This is because at this time, diagnostic testing for the novel coronavirus via real-time RT-PCR is only conducted at the CDC. While our lab may have a PCR for coronavirus, it is not the same subtype as the COVID-19 subtype causing the current epidemic. The state health department will assist you in obtaining the necessary specimens and ensuring proper storage and ideal delivery to the CDC. In fact, the CDC recommends that for biosafety reasons we do not perform our own virus isolation cell cultures or attempt to characterize the viral agent recovered in cultures of specimens from a PUI. To your patients, explain that samples are collected and sent to the CDC to rule out the infection with a turnaround time of two to three days.
Nevertheless, there are other simultaneous diagnostic tests that should be obtained and documented when sending samples to the CDC. The requested panel includes:
- Influenza rapid and PCR
- Parainfluenza
- RSV
- Adenovirus
- Rhinovirus/enterovirus
- Human metanpneumovirus
Most of these should be available as part of our viral panel. Depending on the severity of the respiratory illness, infectious control personnel may request additional specimens that include an NP swab, OP swab, sputum, BAL fluid, tracheal aspirate or stool samples. Until further guidelines are available, work with infectious control employees, ID consultants and the CDC to ensure adequate diagnostic evaluation.
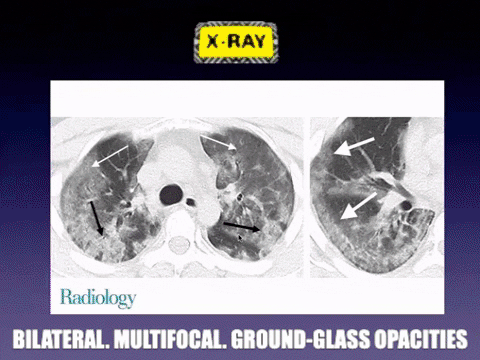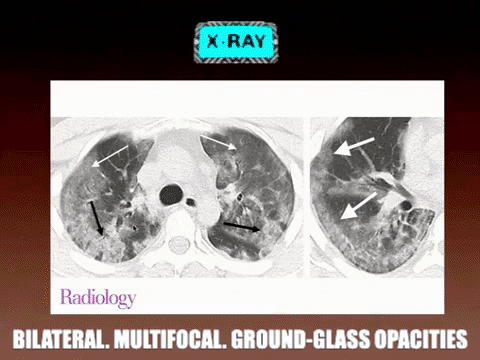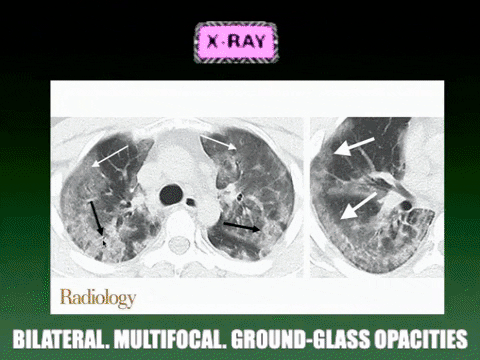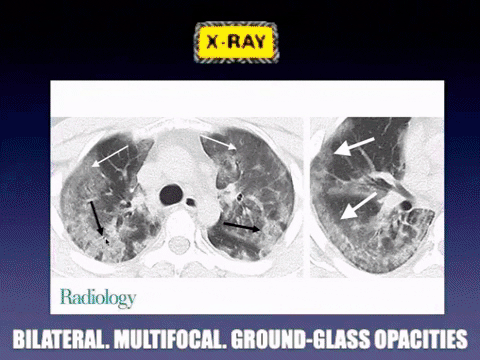
For your own curiosity, there are some some common laboratory and radiographic findings on admission that can be supportive but not specific for the viral illness. These include leukopenia (9–25%), leukocytosis (24–30%), lymphopenia (63%), and elevated alanine aminotransferase and aspartate aminotransferase levels (37%). Most patients will have a normal procalcitonin level and chest CT images usually show bilateral involvement with multifocal consolidation and ground-glass opacities.
What are the necessary isolation precautions?
As soon as you have a person with suspected novel coronavirus infection, ensure adequate precautions that include standard, contact, droplet and eye or face protection. The CDC also recommends initial airborne precautions while the WHO only recommends it necessary when doing aerosol-generating procedures such as non-invasive ventilation, bronchoscopy or CPR. If available, patients with severe respiratory illness should be placed in Airborne infection isolation rooms (AIIRs).
In addition, patients, their families and your colleagues should be educated on the importance of diligent prevention precautions as discussed below.
What are the recommended practices to prevent transmission?
As with most infectious viruses, practices to prevent further exposure by reducing transmission include diligent handwashing, respiratory hygiene and avoiding close contact with ill individuals. Carefully advise families or individuals taking care of those medically stable and being monitored at home that they should wear a medical mask when in the same room as the patient. When at home with someone with a suspected viral illness, clean often, especially things that are touched.
How do you manage patients with suspected infection?
The management schema is broad and based on the severity of illness. For now, there is no direct treatment or vaccine, management is supportive. Supportive care can generally be summarized as follows:
- Oxygenation: provide adequate oxygenation if hypoxic (target SpO2 ≥ 90%). Escalate as necessary in those with severe acute hypoxemic respiratory failure including mechanical ventilation when deemed necessary. The usual pathophysiology of hypoxemia in these patients is usually V/Q mismatch as it is in ARDS.
- Empiric antibiotics: Even though your patient may be suspected to have the novel coronavirus, you still administer appropriate empiric antibacterial coverage for Community or healthcare-associated pneumonia, especially if septic.
- Empiric flu treatment: The WHO also recommends empiric administration of anti-influenza treatment with the respective neuraminidase inhibitor that can be de-escalated once you have confirmed negative microbiology results.
- IV fluids: this might be an initial reflex for those meeting criteria for sepsis but the WHO recommends applying conservative IV fluid administration in those without evidence of shock to as it may worsen oxygenation.
- ICU management: patients presenting with ARDS or septic shock need to be managed in the unit. If presenting with respiratory failure and requiring mechanical ventilation, the WHO presents recommendations almost equivalent to those of managing ARDS including low tidal volumes, lower plateau pressures, proning if necessary and escalation to ECMO as deemed necessary by the intensivist’s expertise. As mentioned above, the details are beyond the scope of this post.
- Steroids: both the WHO and the CDC do not recommend the use of glucocorticoids unless there are other indications such as a COPD exacerbation. This recommendation is based on prior studies of the Middle East Respiratory Syndrome Coronavirus (MERS-CoV) and influenza.
- Investigational treatments: there are active randomized control trials evaluating antiviral treatment targeted towards COVID-19 that are based on a similar nucleotide analogue that was used against SARS and MERS-CoV. These are obviously being done in China and are unlikely to be available for compassionate or investigational use here in the US.
Personally, I found the detailed WHO’s white paper on clinical management of the novel coronavirus pretty useful. Check it out!
In summary…
- Educate your patients on your understanding of the outbreak of the novel coronavirus and why it is a public health emergency. Also explain when you would have suspicion for someone with suspected Coronavirus as outlined by the above CDC criteria.
- Immediately upon suspicion, place the patient under the mentioned infection control precautions, obtain the mentioned respiratory viral panels and notify our infection control personnel who will work with the state health department to obtain the necessary diagnostic testing. Whether they are being managed at home or in the hospital, educate patients and their close contacts on the importance of diligently practicing transmission precautions.
- Provide the necessary supportive care, as outlined above, to patients with acute respiratory illness. Those with mild respiratory illness can be safely managed at home after adequate education to patients and their families on contact and respiratory isolation as outlined above.
References:
- https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-criteria.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fcoronavirus%2F2019-ncov%2Fclinical-criteria.html
- https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-guidance-management-patients.html
- https://www.cdc.gov/coronavirus/mers/infection-prevention-control.html
- https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-guidance-management-patients.html
- https://www.cdc.gov/coronavirus/2019-ncov/lab/guidelines-clinical-specimens.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fcoronavirus%2F2019-ncov%2Fguidelines-clinical-specimens.html
- https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200127-sitrep-7-2019–ncov.pdf
- https://www.who.int/news-room/detail/30-01-2020-statement-on-the-second-meeting-of-the-international-health-regulations-(2005)-emergency-committee-regarding-the-outbreak-of-novel-coronavirus-(2019-ncov)